Obvious in hindsight? – How lifestyle can lower claim cost in oncology and flatten the cost curve by 2030.
Executive Summary
How Food, Movement & Mindset Are Lowering Claims in Oncology: The Data You Need
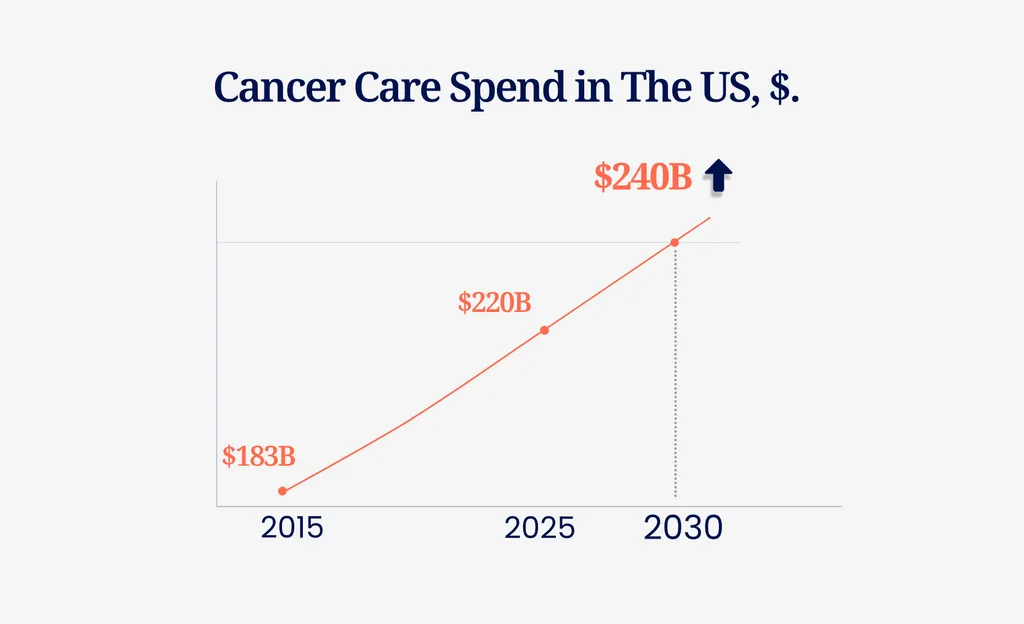
Cancer is among the fastest-growing and most expensive health conditions in the U.S., with total care costs projected to exceed $240 billion by 2030. Yet amid the high-cost treatments and complex care pathways, lifestyle factors like physical activity, nutrition, and weight management are proving to be some of the most powerful tools we have to improve outcomes, and reduce costs.
Still, the healthcare system underutilizes these proven interventions. Only 4% of survivors meet basic lifestyle guidelines according to the American Cancer Society. Targeted lifestyle changes, especially in cancer survivorship, can reshape cost curves, empower patients, and offer a high-value lever for health plans, employers, and providers.
Context: The Cancer Cost Crisis:
A System on the Brink
Cancer is not just a medical diagnosis, it’s a long, challenging and expensive journey. For patients, families, and payers alike, the economic toll is sobering:
- $209 billion was spent on cancer care in the U.S. in 2020. The National Cancer Institute projects that number will exceed $240 billion by 2030 a 34% increase over 2015, outpacing every other cost category aacr.orgnihcm.org.
- Cancer now consumes 7% of U.S. healthcare spending—more than any single disease
For Employers & Health Plans:
- 55–85% of surveyed employers cite cancer as a top 3 cost driver; about 43–55% rank it as the single greatest driver axios.com+11businessgrouphealth.org+11pwc.com+11.
- Costs for employees with cancer are 4–5× higher than those without, and can reach $140 k just for breast cancer treatment fightcancer.org+3color.com+3treatcancer.com+3.
For employers and health plans, cancer is consistently ranked among the top 3 cost drivers, often #1, especially for large self-insured groups, surpassing cardiovascular and musculoskeletal claims in many industries. Costs stem not only from treatment but also from recurrences, late-stage diagnoses, hospitalizations, and long-term disability. As a result claims are not only frequent, they’re high-intensity and persistent over time.
Personal Financial Impact:
Working-age patients often incur $9,000+ in excess annual medical costs, high bankruptcy risk, and long-term wage loss houstonchronicle.com+4jamanetwork.com+4en.wikipedia.org+4. The “financial toxicity” of cancer is real and deadly.

Change: Science Supports Lifestyle-Based Interventions
Amid this financial strain, lifestyle interventions, particularly exercise, offer dramatic benefits:
Multiple meta-studies associate lifestyle to
- 24% lower risk of all-cause mortality
- 33% lower cardiovascular-related mortality
The latest groundbreaking study, the CHALLENGE trial, has established that survival benefits from exercise rival chemotherapy. NEJM trial shows structured exercise over 3 years in colon cancer survivors led to a 37% drop in all-cause mortality and 28% fewer recurrences, compared to education alone wsj.com+1en.wikipedia.org+1.
- AICR Research: Between 30–50% of cancers are preventable through diet, physical activity, and maintaining a healthy weight.
- ASCO Guidelines now recommend routine physical activity and nutrition counseling for survivors.
Biologically, exercise reduces systemic inflammation, improves immune response, and favorably alters tumor microenvironments, rebalance hormones (e.g., insulin, estrogen).
Lifestyle change isn’t just supportive, it has direct therapeutic effects. This isn’t soft medicine. It’s evidence-based oncology, AND it’s cost-effective.

Challenge: Absymally Low Lifestyle Integration
Despite such compelling evidence, lifestyle interventions remain underprescribed and underreimbursed in oncology settings. This gap represents a missed opportunity, both for improving patient outcomes and for reducing total cost of care.
A large cross-sectional study published in JAMA Oncology (2023) revealed that only 4% of U.S. cancer survivors meet all American Cancer Society (ACS) lifestyle recommendations, healthy body weight, adequate physical activity, sufficient fruit/vegetable intake, and alcohol moderation.
(Wang et al., JAMA Oncol, 2023)
Why is such an obvious low hanging fruit still unplucked?
Lifestyle is Underrated and Underserved:
- Clinical inertia: Oncology remains drug-centric. Exercise interventions lack standardized reimbursement, making uptake slow. While billions are spent on precision medicine and novel drugs, little investment goes toward lifestyle-based interventions that could prevent recurrence, reduce complications, and lower financial strain.
- Unserved by Workforce wellness and Fitness Apps: General workforce wellness programs often miss cancer-risk strategies. This is key as cancer patients have truly unique physical, emotional and pschycosocial needs. They need customized programs and supervised execution.
- Coverage gaps: Insurers focus on acute treatment not long-term lifestyle support, despite evidence of reduced relapses and hospitalizations.
Despite the evidence, most oncology care plans still lack structured, reimbursed pathways for nutrition or exercise prescriptions. Survivors often face fatigue, mental health struggles, and risk of recurrence, but receive minimal lifestyle guidance during recovery.
Why is such an obvious low hanging fruit still unplucked?
Given the data, it’s no longer optional, lifestyle optimization is mandatory:


In my experience leading benefits strategy, I’ve seen few solutions that offer this level of personalized support during such a critical time in an employee’s life. Complement 1 stands out by putting people first—while also showing real potential for near-term cost savings. It’s a rare combination.
—Teri Wisness, Former Head of Benefits, Google and Advisor to Complement 1
Complement 1: A Lifestyle Program That Delivers ROI
Case Study: Randomized controlled trial conducted on 158 patients
Intervention:
- Daily Live 1:1 Lifestyle Intervention focussed on customized plans handling 3600+ unique patient scenarios based on cancer type-stage, treatment, side effects and existing lifestyles, delivered by CoActive Coaches
- 45 Minutes of Daily Live Sessions comprising Exercise, Nutrition and Mind-Body Practices such as Meditation and Breathwork


The Path Forward
While cancer therapies continue to evolve, lifestyle intervention is the most underutilized lever in the oncology cost and outcome equation.
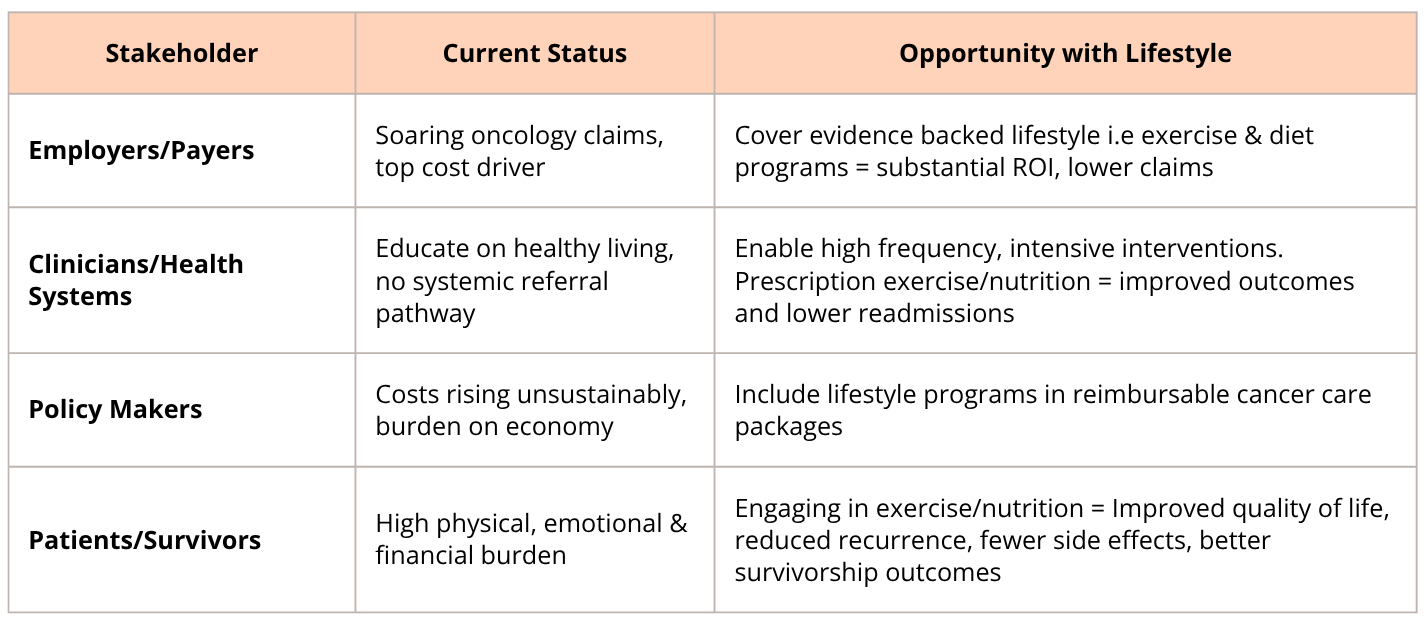
Here’s what needs to happen:
- Employers should integrate lifestyle oncology programs into health benefits
- Health plans must create reimbursement pathways for exercise oncology and nutrition
- Clinicians should routinely prescribe lifestyle just like any other treatment
- Survivors deserve access to evidence-based tools for full recovery, not just remission
Fast Forward to 2030 : 0% increase in cancer costs since 2025, 28% reduced deaths
If even 50% Cancer Patients meet Lifestyle Guidelines, the system can save $20 Bn dollars annually and save 200,000 lives.
- Economic win: Prevented recurrence, lowered hospitalization, reduced disability claims.
- Clinical win: Survival benefits akin to drugs, supported by NEJM and ASCO-level evidence.
- Policy win: Aligns with ACS/AICR guidelines; fills preventive and survivorship care gaps.
The data supports it. The patients want it. And the system needs it.
By prioritizing structured movement, nutrition, and recovery coaching alongside treatment, we don’t just bend the cost curve, we improve quality of life and save human lives.
Author: Trupti Mukker is the Co-Founder and COO of Complement 1, where she leads operations and behavioral design to integrate evidence-based lifestyle interventions into cancer care. With a background in Six Sigma and technology-driven solutions, she brings a sharp focus on innovation and problem-solving. Trupti has deep expertise in building high-impact consumer focussed models at scale. She is passionate about combining science, empathy, and execution to improve health outcomes at scale.



